Suicide kills more men under the age of 50 than anything else. In the UK someone takes their life every 90minutes. Estimated that for every person who dies by suicide twenty more attempt it. Many people who attempt suicide either want to end it all, or some are grateful that they may be unsuccessful attempts. To prevent suicide, we have to intervene early on. But to do this we have to understand how a person gets to the point of suicidal crisis. Everyone goes through things such as bad relationships, guilt over their children, financial or employment crisis etc, and these all can make you relate to suicidal thoughts. Therefore no one is immune to the effects of suicidal thoughts.

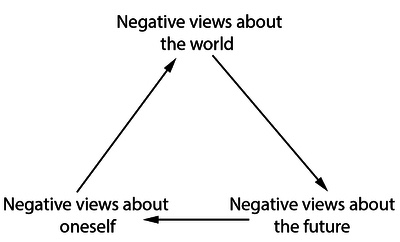
Typically research into the cause of suicide mainly looks into mental illness as the main explanation. It is seen if you have family members whom have a mental illness such as depression etc, or an unstable up-bringing this can make you more susceptible to mental health issues and possibly suicidal ideation. Children as young at 6-7yrs old can experience a first episode of psychosis; auditory or visual hallucinations and paranoid thoughts etc. At this age they often keep it to themselves as they are scared, but this can lead to mental breakdowns. Also other disorders like depression&anxiety or bipolar can occur. This can mean young children will often feel low for periods of time, and if not treated they can develop into suicidal ideations, which they may act upon. Suicidal thoughts don’t just occur for adults who’ve lived a life, it can occur in anyone, at any age. Many people live their life daily, with suicidal ideations, but it’s how they manage these thoughts which is the important point. According to research, people with a mental illness are 30 times more likely to commit suicide than the general population. The Beck’s cognitive triad is often what see occurring in individuals whom struggle with suicidal ideations.
Trying to predict and prevent suicidal attempts is unfortunately heartbreakingly difficult. Even though mental illness is a major factor, many people with a diagnosed mental illness may never have suicidal ideations. A worrying notion is there maybe twice as many people in the general population whom have suicidal thoughts, but aren’t in contact with mental health services. A survey conducted by Men’s Health magazine in November 2017, had 15,000 male responders. 56% admitted to having suicidal thoughts. This does not mean that 56% of the men whom responded are mentally ill. Nonetheless, it highlights that men are struggling with these thoughts, and something needs to change in the current services and society. 70% of the respondents admitted that their own physical health is not good. One conclusion from the survey was, there is a conflict in masculinity; that men today pride themselves in the idea of the “new man”. But men are in general struggling to reconcile that, with the old thought that men are tough and strong. Men identify themselves with their career and this helps with their self esteem. Some men still believe they should be the main breadwinner of the family and struggle to reconcile these ideas together. This can lead to panic, isolation and withdrawal from society. However , despite these difficulties, men aren’t unaware of these issues and the effect upon them. 69% were good at identifying markers in their mental health, family, friends and intervening to help remedy it. Whilst being unable to identify they have an issue and acknowledge it. It is seen, people are aware of the type of services available in the local community, but men often feel unable to approach such services; battling an internal dialogue between the man they feel they should be, compared to the man they want to be. Men often find it harder in general to ask for help than women.
Furthermore trying to understand the cause of suicide, can be difficult as the there are differing rates of suicide across the UK. Interestingly, the northern part of England has the highest suicidal rate. Therefore, can your risk of suicide be linked to where you live or were brought up? Statistics show if you live in the north east, you are 35% more likely to die by suicide than if you live in London. The main reasons for suicide found in the North were attributed to; bereavement, finance and relationships breaking down. But these are not the sole causes. Research shows that individuals within the lowest socio- economic group in the most deprived areas are 10times more likely to die by suicide than those in the highest socio-economic groups in the most affluent areas. Also, if someone doesn’t have protective factors and a strong network of people around them, they are likely to feel alone and isolated, which can lead to suicide. One major factor as a cause of suicide, is if you know of someone who is close to you, that has taken their own life.
Men often feel like they are living a double life; a confident stable person vs someone who is struggling daily with personal issues. Because of this men find it hard to articulate how they are feeling, bottling everything up. It has been found even though more women attempt suicide than men, more men die by suicide compared to women. Research highlights that men use more lethal and life ending methods of suicide than women. Men’s physical pain capacity and tolerance is higher than women. Overtime a males pain tolerance increases overtime. So if men engage in risky behaviours like self harm and experience traumatic events, this may elevate their pain tolerance. Men can become more emotionally isolated than females, as they invest emotionally to a smaller set of people compared to females, whom often have a larger network of support.
However, knowing all these risk factors, it doesn’t help us understand who will take their own life. Therefore without this foresight, it can be difficult in preventing suicidal deaths. Different people require different methods of help. Research looking into the interactions between multiple risk factors and the chance of suicidal death, are able to predict the likelihood of successful/unsuccessful attempts of suicide up to 90% accuracy. This can help us understand when to intervene to prevent suicide. However this is based upon a computer algorithm, which analyses a vast amount of date and factors. Therefore, can a healthcare professional rely solely on a machines diagnosis?
Changing the general populations outlook towards suicide, may help reduce suicidal rates. In America, they have a system where they ask the primary healthcare professional to screen each patient every time they see them, to find out if they have had any suicidal thoughts. Each patient who is seen as a risk is then referred onto the appropriate care/service. In addition, the patient formulates “Rescue Plans” for when they reach crisis point. It was found, that the suicide rate in the local community decreased by 80% and for a few years it was 100% effective, with no suicides reported. If we are more proactive and change the attitude towards suicide, we are more likely to prevent suicidal rates increasing. However, individuals in the lower socio-economic groups who often don’t visit any health services in the US, are still at a higher risk than those whom are able to afford healthcare.
Currently in the UK the governments target is to reduce the deaths by suicide by 10% before 2020. But many believe we should have a bigger goal than 10%. Zero suicidal alliance has the goal of bringing the initiate the US are using of ‘zero suicide’ to the UK. It’s aim is to apply and use the resources we currently have in a more useful way, to prevent people reaching a crisis point. So far nearly all the NHS trusts across the county have signed up for this initiative. However, there is still a lack of funding for research in the mental health sector and for suicide research.
One preventive method in helping others is talking and asking questions like “are you ok?” or “are you suicidal?”. By starting this open conversation, people feel supported and protected. People than feel listened to and their feelings are validated. As small as asking these questions, may save someone’s life.





